This topic uses the AIM Learning Cycle to help MBBS students understand the anatomical organization, development and functional role of salivary glands by integrating Anatomy, Embryology, Physiology and Biochemistry.
1. Curriculum Coverage
Anatomy
• Gross anatomy of parotid gland
• Gross anatomy of submandibular gland
• Gross anatomy of sublingual gland
Embryology
• Development of salivary glands
Physiology
• Secretion of saliva
• Nervous regulation of salivary secretion
• Stimuli increasing salivary secretion
• Plasma and saliva electrolyte composition at different secretion rates
• Function of salivary mucus
• Role of saliva in oral hygiene
• Role of saliva in elimination of heavy metals
. Digestion by salivary amylase (ptyalin)
Biochemistry
• Composition of salivary secretions
• Formation of salivary secretions
• Functions of saliva
📚 Standard Reference Framework
Primary Anatomy Reference:
BD Chaurasia — Standard Undergraduate Depth
Concept Support:
Gray’s Anatomy for Students
Spatial Atlas:
Netter Atlas
Physiology:
Guyton & Hall
Histology:
DiFiore Atlas
Biochemistry:
Lippincott Illustrated Reviews
🎯 Depth Policy
All content is restricted to 2ND Year MBBS Level.
2. Learning Material
1️⃣ Introduction
Salivary glands are essential accessory organs of the digestive system responsible for producing saliva, which maintains oral health and initiates digestion. These glands are located around the oral cavity and include the parotid, submandibular, and sublingual glands. Their secretions help lubricate food, protect teeth, regulate oral hygiene, and facilitate digestion through enzymatic action. Development of salivary glands begins early in embryonic life through epithelial proliferation. Clinically, disorders such as dry mouth (xerostomia), salivary stones, and nerve damage significantly affect digestion and oral health, making this topic highly relevant for clinical understanding.
2️⃣ Foundation Basics
Key Definitions
- Saliva — A watery secretion produced by salivary glands that lubricates food and begins digestion.
- Major Salivary Glands — Parotid, Submandibular, and Sublingual glands.
- Serous secretion — Watery secretion rich in enzymes.
- Mucous secretion — Thick secretion rich in mucin.
- Mixed glands — Glands containing both serous and mucous cells.
- Salivary amylase — Enzyme that initiates carbohydrate digestion.
- Acinus — Secretory unit of salivary gland.
- Duct system — Channels modifying saliva composition.
3️⃣ Core Learning — Curriculum Coverage
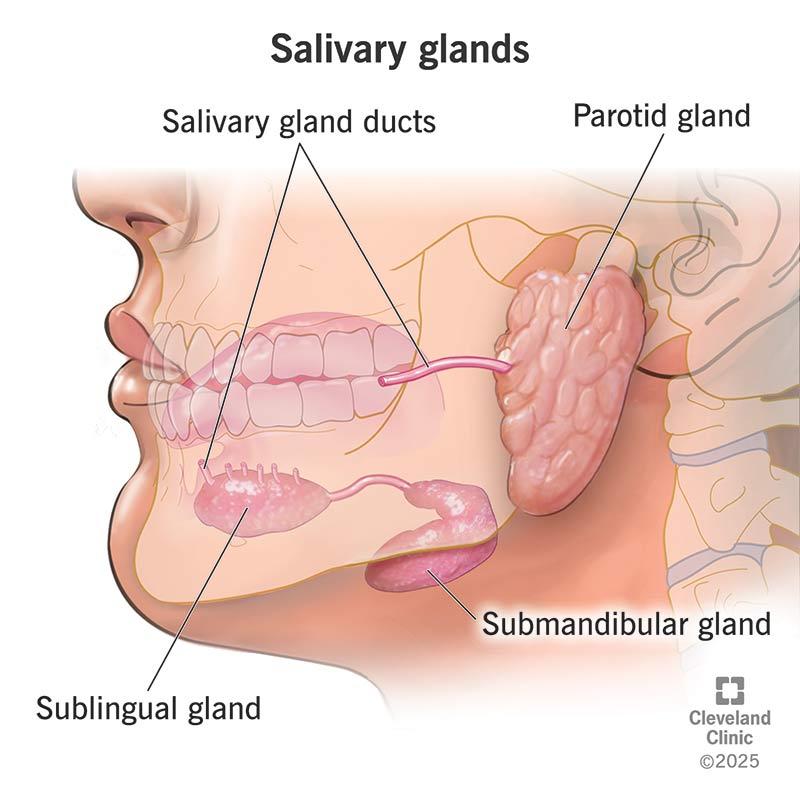
1️⃣ Definition of Major Salivary Glands
• Major salivary glands are large paired exocrine glands that produce saliva.
• They release saliva into the oral cavity through ducts.
• They support digestion, lubrication and oral protection.
✔ Necessary
✔ Non-duplicative
✔ Foundation concept
2️⃣ Names of Major Salivary Glands
• Parotid gland
• Submandibular gland
• Sublingual gland
✔ Mandatory
✔ High-yield
3️⃣ General Location Around Oral Cavity
(Not individual relations)
Explain:
• Parotid — near ear
• Submandibular — below mandible
• Sublingual — floor of mouth
Short only — details later.
✔ Prevents repetition later
✔ Gives spatial orientation
4️⃣ Relative Size of Glands
• Parotid — Largest
• Submandibular — Medium
• Sublingual — Smallest
Faculty expect this comparison.
5️⃣ Type of Secretion (General Comparison)
Very important table.
| Gland | Type of Secretion |
| Parotid | Serous |
| Submandibular | Mixed |
| Sublingual | Mucous dominant |
✔ High-yield
✔ Exam relevant
✔ No duplication later
6️⃣ Duct Names
Just list:
• Parotid → Stensen duct
• Submandibular → Wharton duct
• Sublingual → Ducts of Rivinus
Do NOT describe course yet.
That belongs under each gland.
7️⃣ Contribution to Saliva Production
Very useful overview point.
• Submandibular → Major resting secretion
• Parotid → Active secretion
• Sublingual → Lubrication support
High-yield concept.
8️⃣ Functional Importance of Major Glands
Short list:
• Lubrication
• Digestion
• Protection
• Speech support
Master Concept Map
SALIVARY GLANDS
│
─────────────────────────────────────────────────
│ │ │ │
ANATOMY EMBRYOLOGY PHYSIOLOGY BIOCHEMISTRY
│ │ │ │
Major glands Development Saliva Composition
│ │ Secretion Formation
│ │ Regulation Functions
│ │ Electrolytes Amylase
│ │ Mucus role
│ │ Oral hygiene
│ │ Heavy metal removal
│
Parotid
Submandibular
Sublingual
│
Structure → Duct → Function
│
Clinical Relevance
(Xerostomia, Stones, Parotitis)
SUB-MAP 1: Major Salivary Glands Overview
MAJOR SALIVARY GLANDS
│
─────────────────────────────────────
│ │ │
PAROTID SUBMANDIBULAR SUBLINGUAL
│ │ │
Serous Mixed gland Mucous
│ │ │
Stensen duct Wharton duct Multiple ducts
│ │ │
Upper molar Lingual frenulum Floor of mouth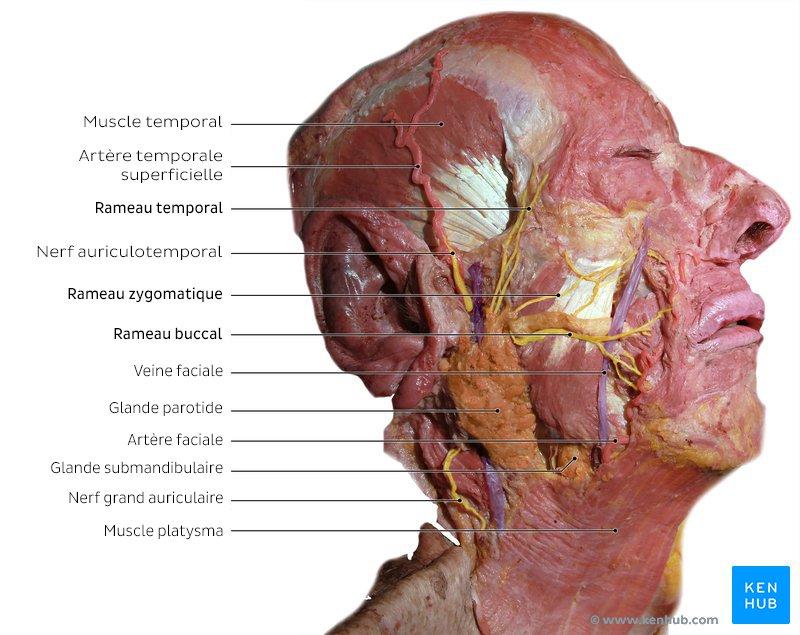
- Structure
- Largest salivary gland
- Located anteroinferior to ear
- Lies between ramus of mandible and sternocleidomastoid muscle
- Enclosed in parotid fascia
- Traversed by facial nerve
- PAROTID DUCT
(Stensen Duct)
Course
Emerges from anterior border
Runs over masseter muscle
Turns medially
Pierces buccinator muscle
Opens into oral cavity
Opening Site
Opposite:
Upper second molar tooth - Blood Supply
- Superficial temporal artery
(Branch of External carotid artery)
Nerve Supply - Glossopharyngeal nerve (CN IX) — Parasympathetic secretion
- Auriculotemporal nerve — Carries secretomotor fibers
Structure → Function - Large serous acini produce watery saliva
- Enables rapid secretion during chewing
Parotid Gland — Important Relations
Lateral: - Skin
- Superficial fascia
- Parotid fascia
Medial: - Ramus of mandible
- Masseter muscle
Anterior: - Mandible
- Masseter
Posterior: - Sternocleidomastoid muscle
- Mastoid process
Contents of Parotid Gland: - Facial nerve
- External carotid artery
- Retromandibular vein
- SURFACES
(Important BD Chaurasia detail)
1️⃣ Superficial Surface
Related to:
• Skin
• Superficial fascia
2️⃣ Anteromedial Surface
Related to:
• Ramus of mandible
• Masseter muscle
3️⃣ Posteromedial Surface
Related to:
• Mastoid process
• Sternocleidomastoid
• Styloid apparatus
4️⃣ Superior Surface (Base)
Related to:
• External acoustic meatus - IF DAMAGED
(Cause → Effect)
Parotid Inflammation
Cause:
Viral infection (e.g., mumps)
Effect:
• Painful swelling
• Reduced salivation
Facial Nerve Injury
Cause:
Parotid surgery
Effect:
• Loss of facial expression
• Facial asymmetry
• Difficulty closing eye
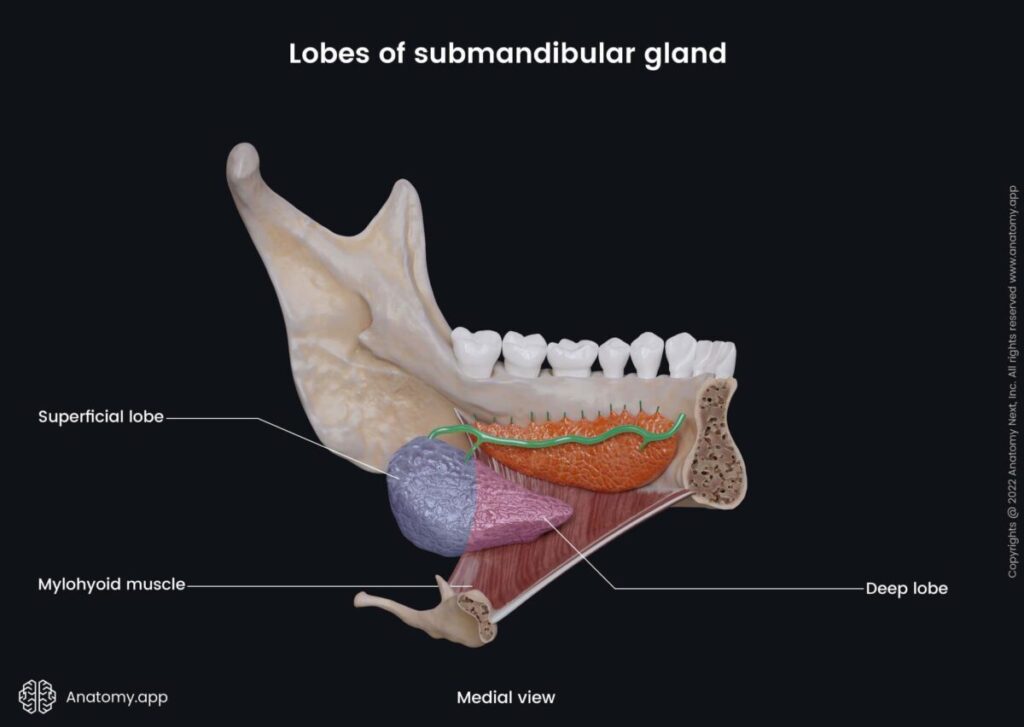
- Structure
- The gland lies in the submandibular triangle.
It consists of:
1️⃣ Superficial Part
• Large portion
• Lies below mandible
• Occupies submandibular triangle
2️⃣ Deep Part
• Small portion
• Extends forward
• Lies in floor of mouth
• Curves around posterior border of mylohyoid muscle
This feature is very characteristic. - Lies medial to mandible
- Mixed gland (serous dominant)
- Wharton duct opens beside lingual frenulum
Blood Supply - Facial artery
Nerve Supply - Facial nerve (via chorda tympani)
Structure → Function - Produces majority of saliva at rest
- Mixed secretion allows lubrication and digestion
Submandibular Gland — Important Relation - Superficial Part Relations
Superior:
• Body of mandible
Inferior:
• Skin
• Platysma
• Deep fascia
Medial:
• Mylohyoid muscle
• Hyoglossus muscle
Lateral:
• Mandible
Deep Part Relations
(Very High Yield)
Related to:
• Hyoglossus muscle
• Lingual nerve
• Submandibular duct
The lingual nerve loops around the duct — clinically important relation. - SUBMANDIBULAR DUCT
(Wharton Duct)
Origin
From:
Deep part of gland
Course
Runs forward in floor of mouth
Lies between:
• Hyoglossus muscle
• Mylohyoid muscle
Crossed by:
Lingual nerve
Opens near:
Lingual frenulum - IF DAMAGED
- (Cause → Effect)
- Submandibular Stone Formation
- (Sialolithiasis)
- Cause:
- Duct obstruction
- Effect:
- • Pain during meals
- • Swelling of gland
- • Reduced salivation
- This gland is most commonly affected by stones.
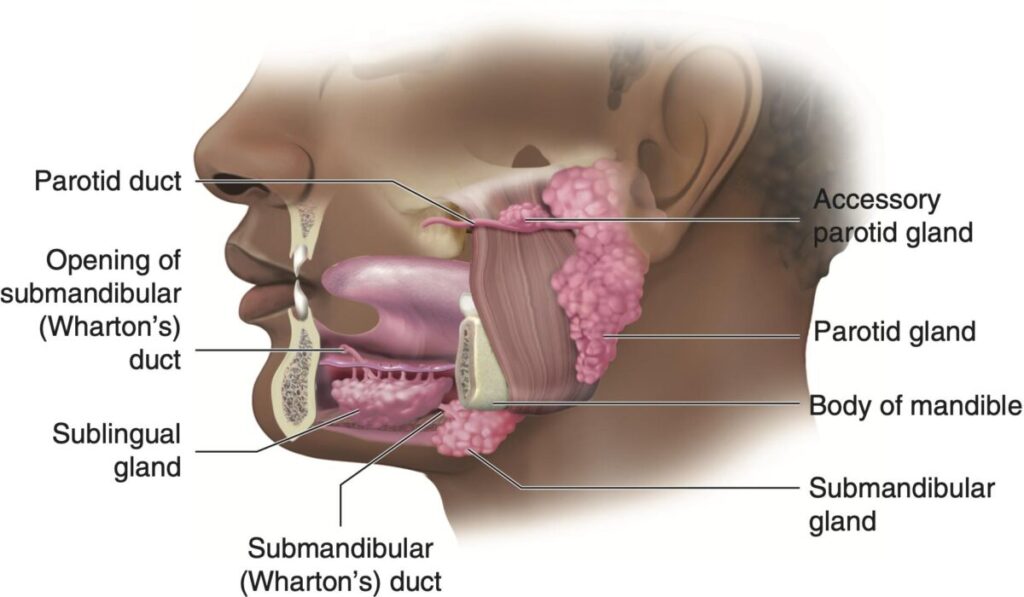
- Structure
- Smallest salivary gland
- Located beneath mucosa of floor of mouth
Blood Supply - Lingual artery
Nerve Supply - Facial nerve (via chorda tympani)
Structure → Function - Produces mucous-rich saliva
- Helps lubrication of oral cavity
- DUCT SYSTEM
Unlike other glands:
• Has multiple ducts
Called:
Ducts of Rivinus
Course of Ducts
• Open directly into floor of mouth
• Open along sublingual fold
Sometimes:
One duct joins:
Submandibular duct
(This variation is acceptable undergraduate level knowledge.)
Sublingual Gland — Relations - The gland lies in the floor of the mouth.
- Position:
- • Superior: Mucous membrane of floor of mouth
- • Inferior: Mylohyoid muscle
- • Medial: Genioglossus muscle
- • Lateral: Mandible
- This shallow position allows direct opening into the oral cavit
- IF DAMAGED
- (Cause → Effect)
- Sublingual Duct Blockage
- Cause:
- Duct obstruction
- Effect:
- • Swelling in floor of mouth
- • Difficulty swallowing
- • Reduced lubrication
🧠 CORE
(High-yield essentials)
- Salivary glands develop from oral ectoderm.
- Development begins as epithelial buds from oral cavity lining.
- Buds grow into underlying mesenchyme.
- The proximal part forms ducts.
- Terminal parts form secretory acini.
- Development occurs at different weeks for each gland.
- Branching produces the lobular structure of glands.
- Functional maturation occurs before birth.
🔬 CONCEPT EXPLAINED
What is the Development of Salivary Glands?
Salivary glands develop from epithelial cells lining the primitive oral cavity. These cells proliferate and form solid epithelial buds that grow into surrounding mesenchyme. With continued growth and branching, these buds form ducts and secretory units that later produce saliva.
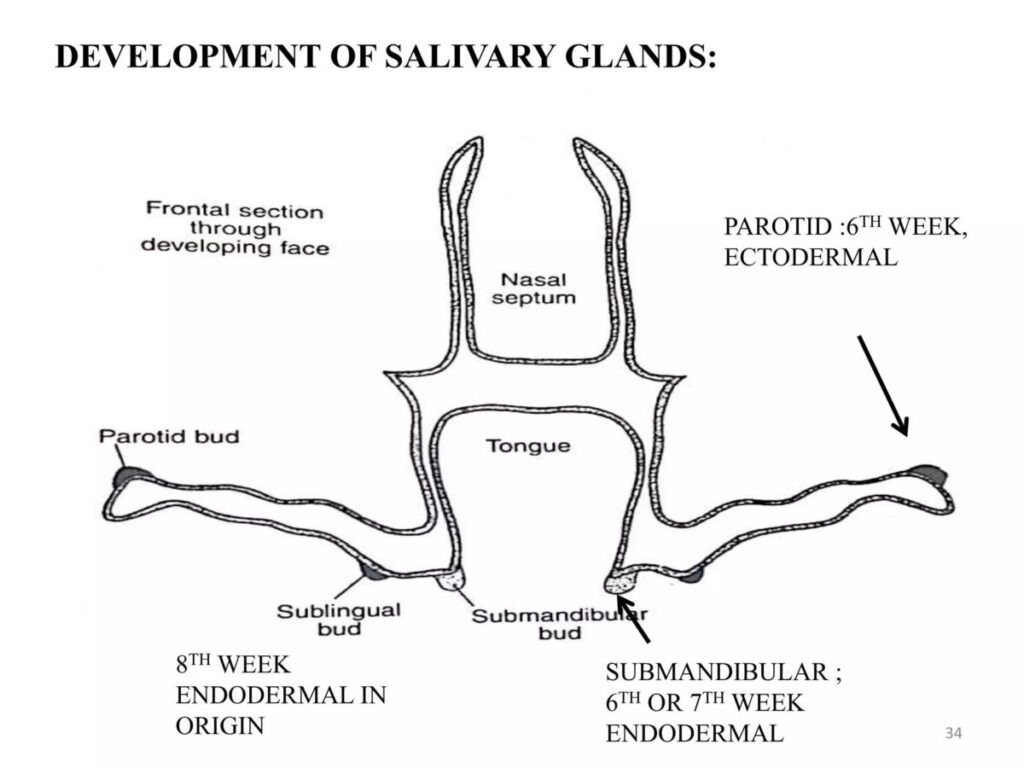
📍 DEVELOPMENTAL ORIGIN
Germ Layer Origin
- Ectoderm of oral cavity
Supporting tissue arises from: - Surrounding mesenchyme
Structure → Adult Link
Oral epithelium → Duct system
Terminal buds → Secretory acini
This explains why salivary glands are exocrine glands.
📍 TIMELINE OF DEVELOPMENT
(Important standard fact)
Parotid Gland
- Begins development around:
6th week of intrauterine life - First major salivary gland to develop.
Submandibular Gland
- Begins development around:
7th week
Sublingual Gland
- Begins development around:
8th week - Last major gland to develop.
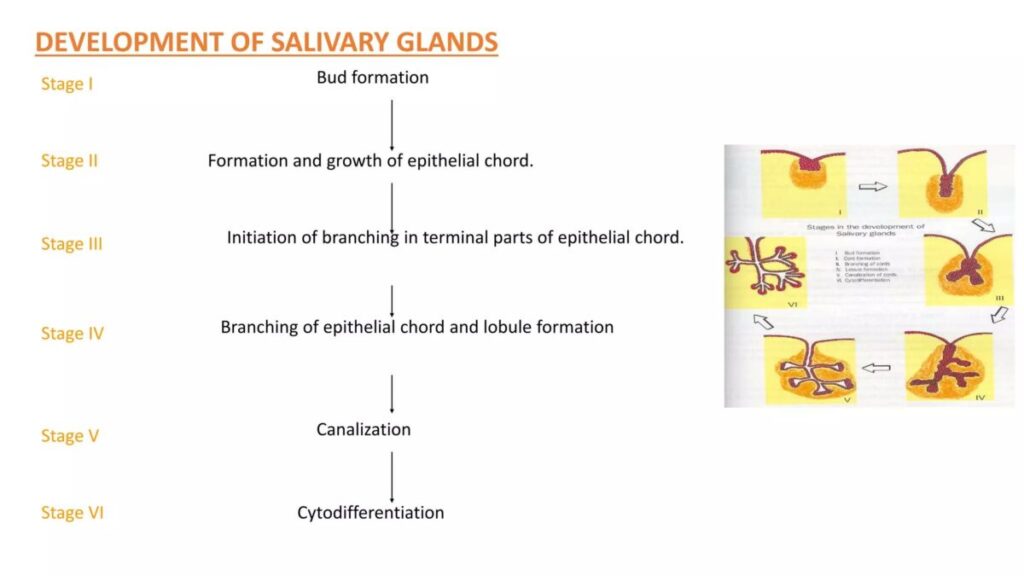
📍 DEVELOPMENTAL STEPS
(Sequential Logic)
Stepwise Mechanism
1️⃣ Oral epithelium thickens
(epithelial placode forms)
↓
2️⃣ Bud formation occurs
(epithelial bud grows)
↓
3️⃣ Bud elongates into mesenchyme
↓
4️⃣ Branching begins
(branching morphogenesis)
↓
5️⃣ Central cells break down
(lumen formation)
↓
6️⃣ Duct system develops
↓
7️⃣ Terminal buds form acini
↓
8️⃣ Gland matures before birth
🔗 STRUCTURE → FUNCTION LINK
Branching development produces:
- Large number of acini
- Increased secretory surface
This supports: - Efficient saliva production
- Functional digestion after birth
⚠️ IF DAMAGED
(Cause → Effect Logic)
Developmental Failure
Cause:
Defective epithelial growth
Effect:
- Absence of gland
- Reduced saliva production
- Difficulty in lubrication
Duct Formation Defect
Cause:
Incomplete canalization
Effect:
- Duct blockage
- Swelling
- Reduced salivary flow
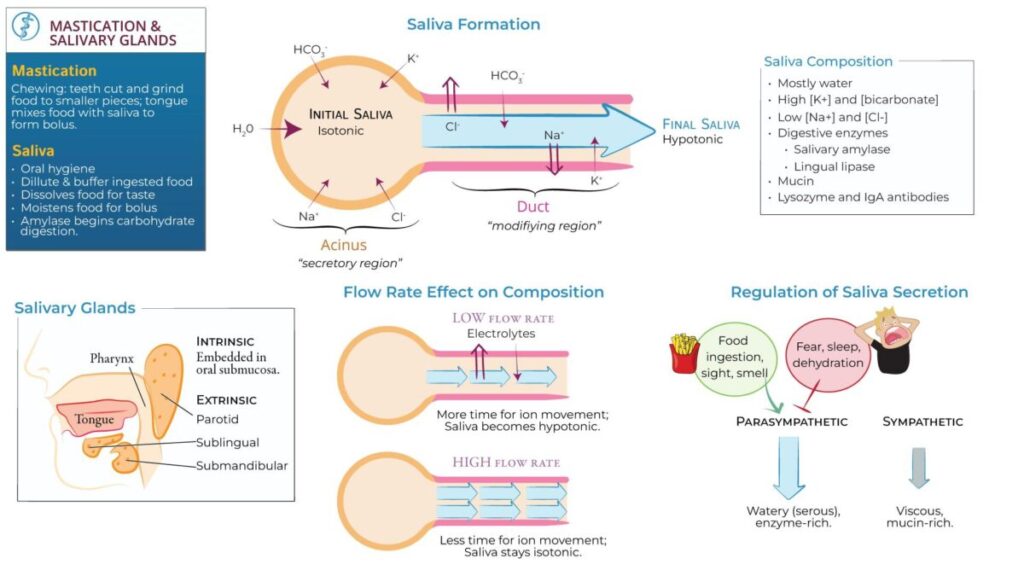
A. Secretion of Saliva
CORE
(High-yield essentials)
- Saliva is secreted by salivary gland acinar cells.
- Initial secretion is called primary saliva.
- Primary saliva is isotonic with plasma.
- As saliva passes through ducts, its composition changes.
- Duct cells modify ion content.
- Final saliva becomes hypotonic.
- Water movement occurs by osmosis.
- Duct permeability to water is low.
🔬 CONCEPT EXPLAINED
What Happens During Saliva Formation?
Saliva formation occurs in two main stages:
1️⃣ Formation of primary secretion
2️⃣ Modification in ducts
These two stages explain how saliva changes from isotonic to hypotonic.
🔄 Mechanism Flow — Formation of Saliva
Stepwise physiological process:
1️⃣ Acinar cells secrete fluid
- Na⁺ actively transported into lumen
- Cl⁻ follows
- Water follows osmotically
Result:
Primary saliva formed (isotonic)
↓
2️⃣ Saliva enters duct system
Duct cells modify ions: - Na⁺ reabsorbed
- Cl⁻ reabsorbed
- K⁺ secreted
- HCO₃⁻ secreted
↓
3️⃣ Water movement limited
Duct walls: - Poor permeability to water
↓
4️⃣ Final saliva formed
Result:
Hypotonic saliva
🔗 Structure → Function Link
Acinar cells → produce fluid
Duct cells → modify composition
Outcome:
Efficient saliva production suitable for digestion and lubrication.
⚙️ B. Nervous Regulation of Salivary Secretion
CORE
- Salivary secretion is controlled by autonomic nervous system.
- Both parasympathetic and sympathetic systems regulate secretion.
- Parasympathetic stimulation produces large volume watery saliva.
- Sympathetic stimulation produces thick mucous saliva.
- Parasympathetic system plays dominant role.
- Reflex control is important.
- Sensory input initiates secretion.
🔬 CONCEPT EXPLAINED
Parasympathetic Control
Parasympathetic stimulation increases:
- Blood flow
- Secretion rate
- Enzyme output
Result:
Watery enzyme-rich saliva
Sympathetic Control
Sympathetic stimulation produces:
- Small amount
- Thick saliva
Result:
Viscous secretion - Salivary Reflex Arc
🔄 Mechanism Flow — Salivary Reflex Arc
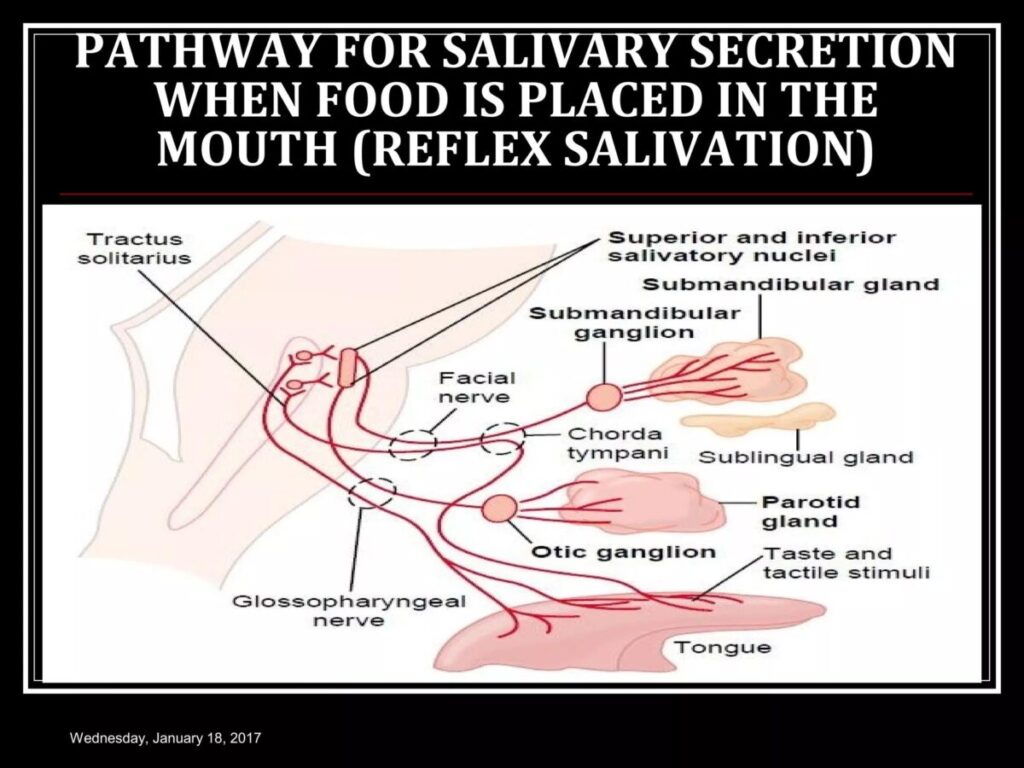
1️⃣ Stimulus Initiation
Food enters oral cavity.
Receptors stimulated:
• Taste receptors
• Tactile receptors
(Afferent limb begins)
2️⃣ Afferent Pathway
Sensory impulses travel via:
• Facial nerve (CN VII)
• Glossopharyngeal nerve (CN IX)
Signals reach:
Salivatory nuclei in medulla
(Control center)
3️⃣ Central Processing
Salivatory nuclei become activated.
Reflex response initiated.
4️⃣ Efferent Pathway
Parasympathetic fibers arise from:
• Superior salivatory nucleus
• Inferior salivatory nucleus
Signals travel to:
Salivary glands.
5️⃣ Effector Activation
Salivary gland cells stimulated.
Blood flow increases.
Secretion increases.
6️⃣ Response
Result:
Increased salivary secretion
Watery enzyme-rich saliva produced.
⚙️ C. Stimuli Increasing Salivary Secretion
CORE
Three major stimuli:
- Taste
- Smell
- Chewing
Other stimuli: - Nausea
- Conditioned reflex
- Thought of food
🔬 CONCEPT EXPLAINED
These stimuli activate sensory receptors that send signals to the brainstem, which in turn activates parasympathetic pathways that increase salivary secretion.
This prepares the digestive system before food enters the stomach.
⚙️ D. Plasma and Saliva Electrolyte Composition
CORE
Electrolyte concentration depends on:
Flow rate
Low flow rate:
- Low Na⁺
- Low Cl⁻
- High K⁺
High flow rate: - High Na⁺
- High Cl⁻
Saliva always remains hypotonic compared to plasma.
🔬 CONCEPT EXPLAINED
At low flow rate, saliva remains longer in ducts.
Result:
More Na⁺ reabsorbed.
At high flow rate, saliva passes quickly.
Result:
Less modification occurs.
⚙️ E. Function of Salivary Mucus
CORE
Mucus provides:
- Lubrication
- Protection
- Cohesion of food
Helps: - Swallowing
- Speech
- Oral protection
🔬 CONCEPT EXPLAINED
Mucus binds food particles into a bolus, making swallowing easier and preventing injury to oral mucosa.
⚙️ F. Role of Saliva in Oral Hygiene
CORE
Saliva supports oral health by:
- Washing away food particles
- Reducing bacterial growth
- Neutralizing acids
- Protecting teeth
🔬 CONCEPT EXPLAINED
Continuous salivary flow prevents accumulation of harmful microorganisms and reduces risk of dental caries.
⚙️ G. Role in Elimination of Heavy Metals
CORE
Saliva helps eliminate:
- Mercury
- Lead
- Certain toxic metals
🔬 CONCEPT EXPLAINED
Toxic substances enter saliva and are removed from the body through swallowing or expectoration.
⚙️ H. Digestion by Salivary Amylase (Ptyalin)
CORE
- Salivary amylase begins carbohydrate digestion.
- Acts on starch.
- Produces maltose and dextrins.
- Works best at neutral pH.
- Activity continues briefly in stomach.
🔬 CONCEPT EXPLAINED
Salivary amylase breaks down complex carbohydrates into smaller sugar molecules during chewing. This early digestion improves efficiency of later digestive processes.
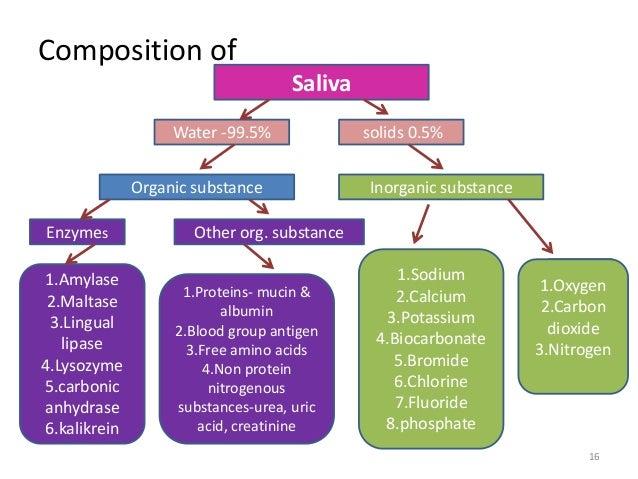
A. Composition of Salivary Secretions
🧠 CORE
(High-yield essentials)
Saliva is composed of:
- Water — about 99%
- Electrolytes
- Proteins and enzymes
- Mucins
- Immunoglobulins
- Antimicrobial substances
- Organic molecules
These components support digestion, lubrication and protection.
🔬 CONCEPT EXPLAINED
Major Components of Saliva
1️⃣ Water (Major Component)
- Forms about 99% of saliva
- Dissolves food substances
- Helps form food bolus
- Facilitates swallowing
Why it exists:
Allows easy movement of food and supports digestion.
2️⃣ Electrolytes
Major ions include:
- Sodium (Na⁺)
- Potassium (K⁺)
- Chloride (Cl⁻)
- Bicarbonate (HCO₃⁻)
Functions: - Maintain ionic balance
- Neutralize acids
- Maintain pH of saliva
- Support enzyme function
3️⃣ Enzymes
(Highly Important)
Major enzymes include:
- Salivary amylase (ptyalin)
- Lysozyme
Functions: - Amylase → Digestion of starch
- Lysozyme → Antibacterial action
Why it exists:
Initiates digestion and protects oral cavity.
4️⃣ Mucins
Mucins are glycoproteins that:
- Provide viscosity
- Lubricate oral cavity
- Protect mucosal surfaces
Structure → Function Link:
Sticky nature allows formation of food bolus.
5️⃣ Immunoglobulins
Major type:
- Secretory IgA
Functions: - Provides immune protection
- Prevents microbial invasion
6️⃣ Antimicrobial Substances
Examples:
- Lysozyme
- Lactoferrin
Functions: - Destroy bacteria
- Maintain oral hygiene
🔗 Structure → Function Link
Chemical composition determines functional ability:
Component Function
Water Lubrication
Electrolytes pH balance
Enzymes Digestion
Mucins Lubrication
IgA Immunity
This relationship is essential for proper salivary function.
🧪 B. Formation of Salivary Components
🧠 CORE
(High-yield essentials)
- Salivary proteins are synthesized in acinar cells.
- Enzymes are produced in rough endoplasmic reticulum (RER).
- Proteins are processed in Golgi apparatus.
- Secretory vesicles store proteins.
- Vesicles release contents into lumen.
- Mucins are synthesized in mucous cells.
- Immunoglobulin A is added to secretion.
🔬 CONCEPT EXPLAINED
Biochemical Formation of Salivary Molecules
Salivary gland cells synthesize proteins such as enzymes, mucins and antimicrobial substances. These molecules are formed through intracellular processes involving protein synthesis and packaging.
Stepwise Biochemical Process
1️⃣ Protein synthesis begins in RER
↓
2️⃣ Proteins transported to Golgi apparatus
↓
3️⃣ Golgi modifies proteins
↓
4️⃣ Proteins packaged into secretory vesicles
↓
5️⃣ Vesicles release contents into lumen
↓
6️⃣ Final secretion contains functional molecules
🔗 Why This Process Exists
This biochemical process allows saliva to contain:
- Digestive enzymes
- Protective proteins
- Lubricating mucins
Without this synthesis, saliva would lack functional capability.
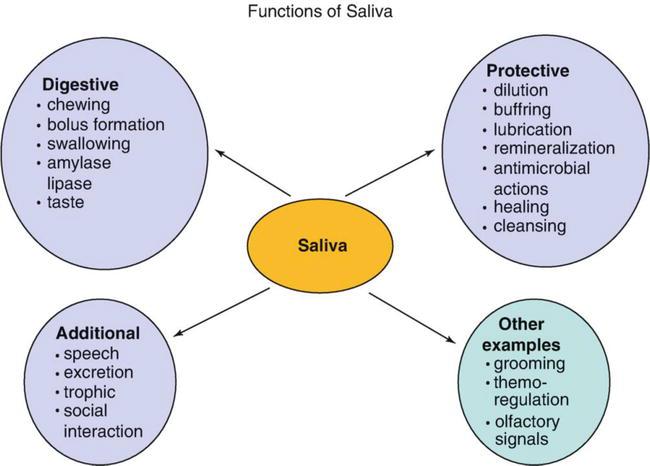
🧪 C. Functions of Saliva
SUB-MAP 3: Functions of Saliva Integration Map
FUNCTIONS OF SALIVA
│
─────────────────────────────────────────
│ │ │ │
DIGESTION LUBRICATION PROTECTION DETOXIFICATION
│ │ │ │
Amylase Mucin IgA Heavy metals
Starch → Swallowing Lysozyme Mercury
Maltose Buffering Lead
Arsenic🧠 CORE
(High-yield essentials)
Major functions include:
- Lubrication
- Digestion
- Protection
- Taste facilitation
- Maintenance of oral health
- Speech support
🔬 CONCEPT EXPLAINED
1️⃣ Lubrication
Mucins coat food particles.
Result:
- Smooth swallowing
- Reduced friction
2️⃣ Digestion
Salivary amylase begins:
- Carbohydrate digestion
Result: - Starch converted into maltose.
3️⃣ Protection
Saliva protects oral tissues by:
- Washing debris
- Neutralizing acids
- Preventing infection
4️⃣ Taste Facilitation
Saliva dissolves:
- Food molecules
Result:
Taste receptors stimulated effectively.
5️⃣ Maintenance of Oral Health
Continuous flow prevents:
- Bacterial accumulation
- Tooth decay
6️⃣ Speech Support
Lubrication allows:
- Smooth tongue movement
- Clear articulation
5️⃣ Functional Integration
Development → Structure → Secretion → Function → Outcome
Stepwise Integrated Functional Chain
Oral ectoderm develops into salivary gland buds
(Embryology)
↓
Branching morphogenesis forms ducts and secretory acini
(Embryology → Anatomy)
↓
Acinar cells produce primary saliva
(Anatomy → Physiology)
↓
Duct system modifies saliva composition
(Physiology)
↓
Saliva contains enzymes, mucus and protective proteins
(Biochemistry)
↓
Final saliva performs essential functions
(Function)
• Lubrication of food
• Initiation of digestion
• Protection of oral cavity
• Maintenance of oral hygiene
↓
Functional Outcome
Efficient:
✔ Chewing
✔ Swallowing
✔ Digestion
✔ Oral protection
6️⃣ Clinical Correlation
Xerostomia (Dry Mouth)
Cause:
- Dehydration
- Nerve damage
- Radiation therapy
Effect: - Difficulty swallowing
- Dental caries
- Oral infections
Sialolithiasis (Salivary Stones)
Cause:
- Calcium deposition in ducts
Effect: - Painful swelling
- Reduced saliva
Parotitis (Mumps)
Cause:
- Viral infection
Effect: - Painful swelling of parotid gland
⭐
7️⃣ Points to Remember
- Parotid gland produces serous secretion
- Submandibular gland produces major resting saliva
- Sublingual gland produces mucous secretion
- Parasympathetic stimulation increases saliva
- Saliva is hypotonic compared to plasma
- Ducts modify electrolyte composition
- Salivary amylase starts starch digestion
- Mucus protects oral mucosa
- Saliva maintains oral hygiene
- Reduced saliva leads to dental caries
Recommended Video
3. PRE-TEST MCQs
Results
#1. Which salivary gland is primarily responsible for producing serous secretion?
#2. The duct of the parotid gland opens into the oral cavity opposite which structure?
#3. Which nerve provides parasympathetic secretomotor supply to the parotid gland?
#4. The submandibular duct opens into the oral cavity near which structure?
#5. Which salivary gland contributes most to resting saliva secretion?
#6. During embryological development, the parotid gland originates from which germ layer?
#7. Which salivary glands develop primarily from endoderm?
#8. The primary stimulus responsible for increased salivary secretion during eating is:
#9. Parasympathetic stimulation of salivary glands typically produces:
#10. Which electrolyte concentration is typically lower in saliva than in plasma at low secretion rates?
#11. The principal function of mucin in saliva is:
#12. Which component of saliva contributes most directly to antibacterial activity?
#13. Which ion is secreted into saliva by duct cells during saliva modification?
#14. During high salivary flow rates, saliva composition becomes more similar to:
#15. Salivary amylase primarily acts on which substrate?
#16. Which of the following best explains the role of saliva in oral hygiene?
#17. Which heavy metal is known to be eliminated partially through salivary secretion?
#18. Which cells are primarily responsible for the formation of primary saliva?
#19. Which structural feature allows duct cells to modify electrolyte composition of saliva?
#20. Damage to salivary glands most directly results in which functional disturbance?
4. Diagnostic Feedback
Your score in this pre-test reflects your current level of understanding of the topic.
Score 0–7 → Foundational Level
You may not yet be familiar with the basic concepts of connective tissue structure and biochemistry.
Focus on understanding the components of extracellular matrix, collagen structure, glycosaminoglycans, and proteoglycans before attempting more advanced questions.
Score 8–14 → Developing Understanding
You have a partial understanding of connective tissue components and their functions.
Review the relationships between collagen fibers, extracellular matrix proteins, and ground substance, and how these components contribute to tissue strength and elasticity.
Score 15–20 → Strong Conceptual Base
You already have a solid understanding of connective tissue biochemistry and structure.
As you proceed through the learning material, focus on integrating histological structure with biochemical mechanisms and physiological functions.
5. Guided Reasoning
Ask AIM Tutor
🧠 Need Help Understanding Incorrect Answers?
I answered this MCQ incorrectly in my MBBS learning module.
Please help me understand:
1. What concept is being tested in this question?
2. Why is the correct option correct?
3. Why are the other options incorrect?
4. What is the key concept I should remember for exams?
Here is the MCQ:
6. Concept Integration
1️⃣ MASTER INTEGRATION CHAIN
Whole Topic Core Flow (Normal → Failure → Drug Action)
Salivary Glands (Parotid, Submandibular, Sublingual)
│
Embryological Development
(Ectoderm / Endoderm → Branching → Acini + Ducts)
│
Normal Structure Formation
(Acini → Secretion | Ducts → Ion Modification)
│
Neural Stimulation
(Taste/Smell → Medulla → Parasympathetic Nerves)
│
Saliva Production
(Water + Electrolytes + Mucin + Amylase + IgA)
│
Functional Outcomes
Lubrication + Digestion + Oral Protection + Detoxification
│
Failure Points
↓
Nerve Damage → Reduced Secretion → Xerostomia
Duct Obstruction → Salivary Stasis → Stones
Acinar Damage → Reduced Enzymes → Poor Digestion
│
Drug Action Points
↓
Parasympathomimetics → Increase Secretion
Anticholinergic Drugs → Reduce Secretion
Artificial Saliva → Restore Lubrication
3️⃣ CORE MECHANISM INTEGRATION
Main Functional Failure — Xerostomia Mechanism
Parasympathetic Failure
(or gland damage / dehydration)
│
Reduced Acinar Stimulation
│
Reduced Primary Saliva Formation
│
Reduced Mucin + Amylase + Electrolytes
│
Loss of Lubrication + Reduced Buffering
│
Functional Breakdown
↓
Difficulty Swallowing
Increased Dental Caries
Oral Mucosal Injury
Reduced Digestion of Starch
Clinical Meaning:
Most salivary disorders produce dry mouth first, followed by oral infections and swallowing difficulty.
4️⃣ CLINICAL INTEGRATION SNAPSHOT
Clinical Flow 1 — Xerostomia (Dry Mouth)
Cause:
Radiation Therapy / Anticholinergic Drugs
│
Mechanism:
Parasympathetic inhibition → Reduced saliva secretion
│
Functional Effect:
Loss of lubrication + Reduced antimicrobial protection
│
Symptoms:
Dry mouth
Difficulty swallowing
Increased dental caries
│
Treatment:
Artificial saliva
Parasympathomimetic drugs
(Hydration support)
Clinical Flow 2 — Sialolithiasis (Salivary Stones)
Cause:
Mineral deposition in salivary duct
│
Mechanism:
Duct obstruction → Saliva stagnation
│
Functional Effect:
Pressure build-up inside gland
│
Symptoms:
Pain during meals
Gland swelling
Reduced saliva flow
│
Treatment:
Hydration
Massage
Stone removal if persistent
Clinical Flow 3 — Parotitis (Mumps Infection)
Cause:
Viral infection of parotid gland
│
Mechanism:
Inflammation → Acinar cell damage
│
Functional Effect:
Reduced saliva secretion
│
Symptoms:
Painful parotid swelling
Fever
Difficulty chewing
│
Treatment:
Supportive therapy
Hydration
Pain management
5️⃣ ULTRA–HIGH–YIELD MASTER SUMMARY
Final Revision Model (Last-Day Memory Tool)
NORMAL SYSTEM
Parasympathetic Stimulation
↓
Acinar Secretion
(Isotonic Fluid)
↓
Duct Modification
(Hypotonic Saliva)
↓
Functional Saliva
Lubrication + Digestion + Protection
DISEASE MECHANISM
Nerve Damage / Duct Block / Gland Injury
↓
Reduced Saliva
↓
Dry Mouth (Xerostomia)
↓
Dental Caries + Dysphagia + Infection
DRUG ACTION
Parasympathomimetics
↑ Saliva
Anticholinergics
↓ Saliva
Artificial Saliva
Restores lubrication
MCQ 1
Question:
A 25-year-old patient develops facial weakness following surgery for a parotid gland tumor. Which structure within the gland is most likely responsible for the observed facial muscle paralysis?
Options:
A. External carotid artery
B. Retromandibular vein
C. Facial nerve
D. Auriculotemporal nerve
E. Posterior auricular artery
Correct Answer:
C. Facial nerve
Explanation:
The facial nerve passes through the parotid gland and controls muscles of facial expression, so injury leads to facial paralysis.
MCQ 2
Question:
A patient complains of painful swelling beneath the mandible that worsens during meals. Imaging reveals obstruction of a duct running forward and opening near the lingual frenulum. Which gland is most likely affected?
Options:
A. Parotid gland
B. Sublingual gland
C. Minor salivary gland
D. Submandibular gland
E. Buccal gland
Correct Answer:
D. Submandibular gland
Explanation:
The submandibular duct (Wharton duct) opens near the lingual frenulum and is commonly affected by salivary stones.
MCQ 3
Question:
A researcher studies salivary secretion and notes that the final saliva produced is hypotonic compared to plasma. Which mechanism is primarily responsible for this change?
Options:
A. Increased water permeability of ducts
B. Active secretion of sodium into ducts
C. Reduced reabsorption of potassium
D. Reabsorption of sodium and chloride without water
E. Passive diffusion of bicarbonate into plasma
Correct Answer:
D. Reabsorption of sodium and chloride without water
Explanation:
Duct cells reabsorb Na⁺ and Cl⁻ but are relatively impermeable to water, producing hypotonic saliva.
MCQ 4
Question:
A newborn is found to have underdeveloped salivary glands due to defective branching of epithelial buds during embryogenesis. Which developmental process was most likely affected?
Options:
A. Canalization of ducts
B. Neural crest migration
C. Branching morphogenesis
D. Differentiation of mesenchyme
E. Formation of mucosal epithelium
Correct Answer:
C. Branching morphogenesis
Explanation:
Salivary glands develop through branching morphogenesis that increases the number of secretory units.
MCQ 5
Question:
During mastication, increased salivary flow is observed when food stimulates oral receptors. Which structure acts as the central control center for this reflex?
Options:
A. Hypothalamus
B. Salivatory nuclei in medulla
C. Cerebellum
D. Thalamus
E. Motor cortex
Correct Answer:
B. Salivatory nuclei in medulla
Explanation:
Salivatory nuclei in the medulla coordinate parasympathetic output to salivary glands.
MCQ 6
Question:
A patient presents with swelling beneath the tongue caused by blockage of multiple small ducts opening along the sublingual fold. Which gland is most likely involved?
Options:
A. Parotid gland
B. Submandibular gland
C. Sublingual gland
D. Lingual gland
E. Minor palatine gland
Correct Answer:
C. Sublingual gland
Explanation:
The sublingual gland has multiple ducts (ducts of Rivinus) opening into the sublingual fold.
MCQ 7
Question:
During salivary secretion, increased flow rate results in higher concentrations of sodium and chloride in saliva. What is the most likely explanation?
Options:
A. Increased secretion of potassium
B. Reduced modification time in ducts
C. Increased water absorption
D. Enhanced bicarbonate removal
E. Increased enzyme secretion
Correct Answer:
B. Reduced modification time in ducts
Explanation:
High flow rate reduces time for Na⁺ and Cl⁻ reabsorption, increasing their concentration.
MCQ 8
Question:
A patient suffering from severe dry mouth shows decreased levels of immunoglobulin A in saliva. Which functional role of saliva is most affected?
Options:
A. Taste sensation
B. Enzymatic digestion
C. Acid neutralization
D. Antimicrobial defense
E. Bolus formation
Correct Answer:
D. Antimicrobial defense
Explanation:
IgA protects mucosa by preventing microbial colonization.
MCQ 9
Question:
During development of salivary glands, epithelial buds grow into surrounding tissue derived from mesenchyme. Which germ layer primarily gives rise to the glandular epithelium?
Options:
A. Endoderm
B. Mesoderm
C. Neural crest
D. Ectoderm
E. Intermediate mesoderm
Correct Answer:
D. Ectoderm
Explanation:
Salivary glands originate from oral ectoderm.
MCQ 10
Question:
A patient exhibits reduced salivary secretion following damage to parasympathetic fibers supplying the submandibular gland. Which nerve pathway is most likely affected?
Options:
A. Glossopharyngeal nerve via otic ganglion
B. Facial nerve via chorda tympani
C. Trigeminal nerve via mandibular branch
D. Hypoglossal nerve via lingual branch
E. Vagus nerve via pharyngeal plexus
Correct Answer:
B. Facial nerve via chorda tympani
Explanation:
Submandibular gland receives parasympathetic supply via chorda tympani of facial nerve.
MCQ 11
Question:
A patient undergoing parotid gland surgery develops loss of salivary secretion from the gland but retains facial muscle function. Injury to which structure is most likely responsible?
Options:
A. Facial nerve trunk
B. Auriculotemporal nerve
C. External carotid artery
D. Retromandibular vein
E. Greater auricular nerve
Correct Answer:
B. Auriculotemporal nerve
Explanation:
Auriculotemporal nerve carries postganglionic parasympathetic fibers to the parotid gland, controlling secretion.
MCQ 12
Question:
A patient presents with difficulty swallowing dry food due to reduced mucous secretion from salivary glands. Which type of secretory unit is primarily responsible for producing mucus?
Options:
A. Serous acini
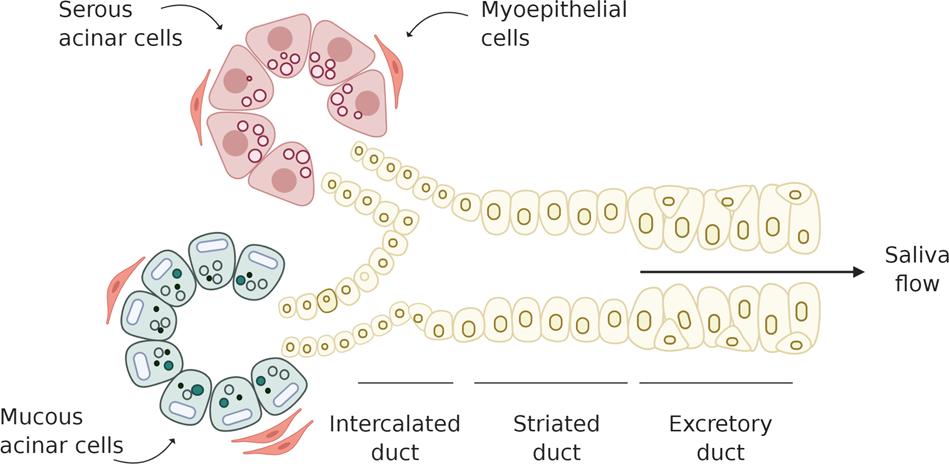
B. Mixed acini
C. Intercalated ducts
D. Mucous acini
E. Striated ducts
Correct Answer:
D. Mucous acini
Explanation:
Mucous acini secrete mucins that lubricate food and facilitate swallowing.
MCQ 13
Question:
A physiology experiment demonstrates that parasympathetic stimulation increases blood flow to salivary glands before secretion begins. What is the primary functional significance of this vascular change?
Options:
A. Reduction of osmotic pressure
B. Supply of nutrients and fluid for secretion
C. Prevention of enzyme degradation
D. Maintenance of ductal pressure
E. Regulation of mucin viscosity
Correct Answer:
B. Supply of nutrients and fluid for secretion
Explanation:
Increased blood flow provides water and electrolytes required for saliva formation.
MCQ 14
Question:
During embryological development, failure of canalization of epithelial cords may result in duct obstruction. What would be the most likely structural consequence of this defect?
Options:
A. Absence of gland capsule
B. Formation of retention cyst
C. Failure of nerve supply
D. Loss of gland vascularization
E. Incomplete epithelial differentiation
Correct Answer:
B. Formation of retention cyst
Explanation:
Failure of duct canalization leads to accumulation of secretions, forming cystic swellings.
MCQ 15
Question:
A patient presents with decreased bicarbonate concentration in saliva. Which functional property of saliva is most likely to be affected?
Options:
A. Digestion of carbohydrates
B. Lubrication of oral mucosa
C. Neutralization of oral acids
D. Activation of taste receptors
E. Formation of food bolus
Correct Answer:
C. Neutralization of oral acids
Explanation:
Bicarbonate buffers acids and maintains oral pH.
MCQ 16
Question:
A physiologist observes that stimulation of sympathetic fibers produces small volumes of thick saliva. Which biochemical component contributes most to the increased viscosity?
Options:
A. Amylase
B. Electrolytes
C. Mucins
D. Immunoglobulins
E. Bicarbonate
Correct Answer:
C. Mucins
Explanation:
Mucins are glycoproteins responsible for the viscous nature of saliva.
MCQ 17
Question:
A patient with prolonged salivary gland dysfunction develops frequent dental caries. Loss of which salivary component most directly contributes to this condition?
Options:
A. Sodium ions
B. Chloride ions
C. Immunoglobulin A
D. Potassium ions
E. Calcium ions
Correct Answer:
C. Immunoglobulin A
Explanation:
IgA protects oral mucosa from bacterial colonization.
MCQ 18
Question:
During feeding, tactile stimulation of the oral mucosa results in salivation even before swallowing begins. Which type of physiological response best explains this phenomenon?
Options:
A. Hormonal secretion
B. Conditioned reflex
C. Simple reflex arc
D. Voluntary motor response
E. Local glandular response
Correct Answer:
C. Simple reflex arc
Explanation:
Salivation occurs through reflex activation of salivatory nuclei following sensory stimulation.
MCQ 19
Question:
A researcher studying saliva observes increased potassium concentration compared to plasma levels. Which physiological mechanism accounts for this finding?
Options:
A. Active secretion of potassium by duct cells
B. Passive diffusion from plasma
C. Increased acinar permeability
D. Reduced sodium reabsorption
E. Increased chloride retention
Correct Answer:
A. Active secretion of potassium by duct cells
Explanation:
Duct cells actively secrete potassium into saliva.
MCQ 20
Question:
A child presents with delayed development of salivary glands. Failure of which early developmental event would most directly impair gland formation?
Options:
A. Neural crest migration
B. Mesenchymal condensation
C. Epithelial bud formation
D. Vascular invasion
E. Nerve differentiation
Correct Answer:
C. Epithelial bud formation
Explanation:
Salivary glands originate from epithelial buds arising from oral ectoderm.
8. Post-Test
Post Test MCQs
9. Explanation of Incorrect Answers
Incorrect answers are valuable learning opportunities. When reviewing MCQs, focus on understanding the concept behind the question, not just memorizing the correct option.
If you answered a question incorrectly:
• Identify the concept being tested.
• Determine why the correct option is correct.
• Understand why the other options are incorrect.
You can paste the MCQ into the AIM Tutor and ask for a step-by-step explanation. This helps strengthen conceptual understanding and improves reasoning for future questions.
Learning Tip
If your Post-Test score is below 80%, review the key concepts and attempt the Post-Test again to reinforce your understanding.
10. Student Memory Support
1️⃣ High-Yield Flashcards
Flashcard 1
Q: Which salivary gland is purely serous?
A: Parotid gland
Flashcard 2
Q: Which gland produces most resting saliva?
A: Submandibular gland
Flashcard 3
Q: Which gland mainly produces mucous secretion?
A: Sublingual gland
Flashcard 4
Q: Which nerve provides parasympathetic supply to parotid gland?
A: Glossopharyngeal nerve (CN IX)
Flashcard 5
Q: Where does parotid duct open?
A: Opposite upper second molar
Flashcard 6
Q: Which cells form primary saliva?
A: Acinar cells
Flashcard 7
Q: Why is final saliva hypotonic?
A: Ducts reabsorb Na⁺ and Cl⁻ but are impermeable to water
Flashcard 8
Q: Which enzyme begins carbohydrate digestion?
A: Salivary amylase
Flashcard 9
Q: Which ion provides buffering action in saliva?
A: Bicarbonate (HCO₃⁻)
Flashcard 10
Q: Which component provides lubrication in saliva?
A: Mucin
Flashcard 11
Q: Which substance provides antibacterial protection in saliva?
A: Lysozyme
Flashcard 12
Q: What happens to sodium level in saliva at high flow rate?
A: Sodium concentration increases
Flashcard 13
Q: Which heavy metals can be eliminated in saliva?
A: Mercury, Lead, Arsenic
Flashcard 14
Q: From which germ layer does parotid gland develop?
A: Ectoderm
2️⃣ Mnemonics
Mnemonic Title:
Contents of Parotid Gland
Mnemonic Word:
“N V A”
Meaning:
N → Facial Nerve
V → Retromandibular Vein
A → External carotid Artery
(Superficial → Deep)
Mnemonic Title:
Major Salivary Glands (Largest to Smallest)
Mnemonic Word:
“Please Send Samples”
Meaning:
P → Parotid
S → Submandibular
S → Sublingual
Mnemonic Title:
Major Salivary Ducts
Mnemonic Word:
“PSR”
Meaning:
P → Parotid → Stensen duct
S → Submandibular → Wharton duct
R → Sublingual → Rivinus ducts
3️⃣ Memory Tables
Table 1 — Major Salivary Glands Comparison
| Feature | Parotid | Submandibular | Sublingual |
|---|---|---|---|
| Type | Serous | Mixed | Mucous |
| Size | Largest | Medium | Smallest |
| Duct | Stensen duct | Wharton duct | Multiple ducts |
| Opening | Upper 2nd molar | Lingual frenulum | Floor of mouth |
| Function | Watery saliva | Resting saliva | Lubrication |
Table 2 — Saliva Formation Stages
| Stage | Site | Main Event |
|---|---|---|
| Primary | Acini | Isotonic fluid formed |
| Secondary | Ducts | Na⁺ reabsorbed, K⁺ secreted |
| Final | Oral cavity | Hypotonic saliva |
4️⃣ Rapid Revision Points
(Last-Minute Revision)
Must Remember:
- Parotid gland contains facial nerve branches
- Submandibular gland produces most resting saliva
- Sublingual gland mainly produces mucous
- Parasympathetic stimulation increases saliva
- Saliva becomes hypotonic in ducts
- Bicarbonate buffers acids
- Mucin lubricates food
- Lysozyme provides antibacterial protection
- Amylase starts starch digestion
- Reduced saliva causes dental caries
- High flow → saliva resembles plasma
5️⃣ Clinical Memory Hooks
Clinical Hook 1:
Xerostomia → Reduced saliva → Difficulty swallowing dry food
Clinical Hook 2:
Parotid surgery → Facial nerve injury → Facial muscle weakness
Clinical Hook 3:
Sialolithiasis → Duct obstruction → Pain during meals
Clinical Hook 4:
Radiation therapy → Acinar damage → Dry mouth
Clinical Hook 5:
Low bicarbonate → Acid damage → Dental caries
✔ Topic Completion
📊 Your Performance
Pre-Test: Not Attempted
Post-Test: Not Attempted
Improvement: --




